Cosmetic Periodontal Treatment in Memphis TN
Periodontal Treatment in Memphis & Collierville TN
OR CALL (901) 761-3770
New & Existing
Patient Forms
PHone
(901) 761-3770
Address
6268 Poplar Ave.
Memphis, TN, 38119
1122 Poplar View Ln N
Collierville, TN 38017


Bite Therapy
Bite therapy focuses on correcting bite issues that contribute to periodontal disease and other oral health problems. This treatment involves adjusting and aligning the bite using techniques such as reshaping tooth surfaces, orthodontic appliances, or custom bite splints. By distributing the forces of biting evenly across all teeth, bite therapy reduces stress on individual teeth and supporting structures, alleviating symptoms like excessive wear and jaw pain, and improving overall oral health.
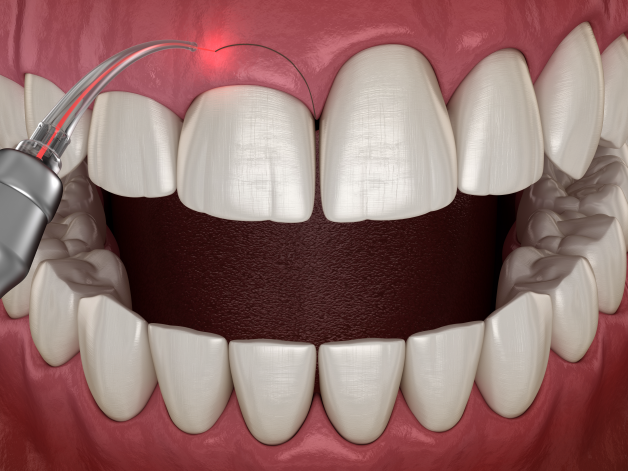
Gingivectomy
A gingivectomy is a surgical procedure used to remove excess gum tissue, often recommended for patients with severe gum disease or for cosmetic purposes. Our periodontists carefully remove and reshape the gum tissue to eliminate pockets that harbor bacteria and improve the aesthetics of the smile. This procedure can be performed using traditional surgical methods or advanced laser technology, resulting in healthier gum tissue and an enhanced appearance.
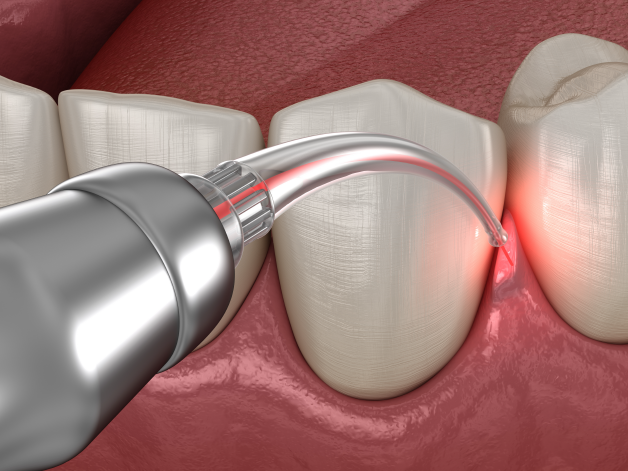
Laser Periodontal Treatment (LANAP)
Laser-Assisted New Attachment Procedure (LANAP) is a cutting-edge treatment for periodontal disease that uses laser technology to target and eliminate diseased tissue while preserving healthy gum tissue. This minimally invasive procedure reduces discomfort and recovery time compared to traditional surgery, promoting faster healing and reducing the risk of infection.
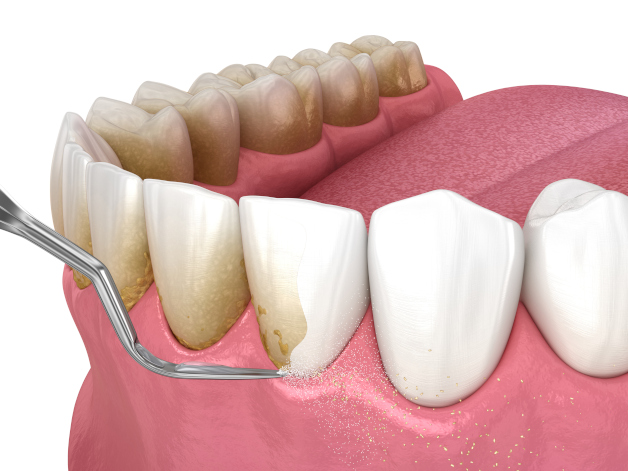
Scaling and Root Planing
Scaling and root planing is a deep cleaning procedure that removes plaque and tartar from below the gum line, effectively treating early-stage periodontal disease. Scaling removes plaque and tartar from tooth surfaces and beneath the gums, while root planing smooths the root surfaces to make it more difficult for bacteria to adhere. This procedure helps reduce gum inflammation and promotes healing.
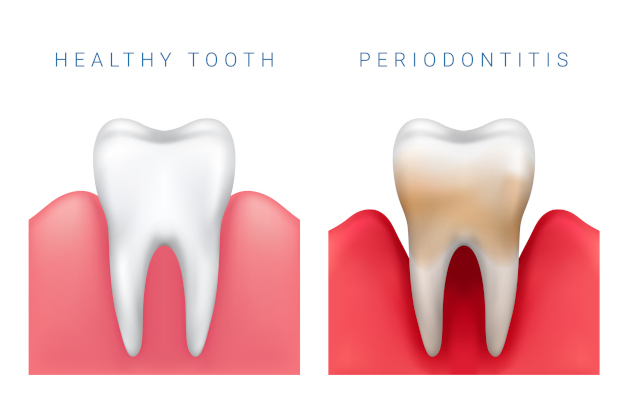
Oral Pathology
Oral pathology involves the diagnosis and treatment of diseases affecting the mouth, including the gums, teeth, and other oral tissues. This field encompasses the study and diagnosis of conditions such as oral cancer, cysts, and other lesions. Regular examinations and biopsies, if necessary, are essential for identifying and treating these conditions early, ensuring overall oral health.

Oral Hygiene
Maintaining good oral hygiene is the foundation of preventing periodontal disease and ensuring overall oral health. Daily practices such as brushing, flossing, and using mouthwash to remove plaque, along with regular dental check-ups and professional cleanings, are essential for keeping gums and teeth healthy. Proper oral hygiene prevents gum disease and tooth decay, promotes fresh breath, and maintains overall oral health.
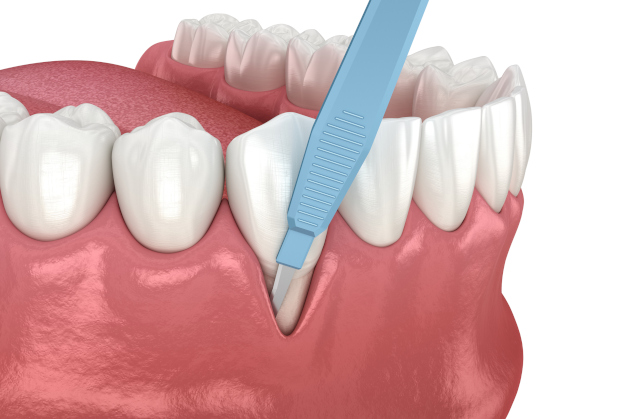
Osseous Surgery
Osseous surgery, also known as pocket reduction surgery, treats advanced periodontal disease by reshaping the bone and gum tissue to eliminate pockets and reduce infection. During the procedure, our periodontists fold back the gum tissue to remove disease-causing bacteria and smooth the damaged bone surfaces, allowing the gum tissue to reattach securely to healthy bone.

Periodontal Maintenance
Periodontal maintenance is an ongoing program designed to prevent the recurrence of periodontal disease after initial treatment. This preventive approach includes thorough cleanings, examinations, and monitoring of the gums and teeth, helping to catch any signs of disease early and maintain oral health. Regular visits to our practice are essential for maintaining healthy gums and supporting structures.

Sedation Dentistry
Sedation dentistry offers a way to make dental treatments more comfortable and manageable for patients who experience anxiety or discomfort during procedures. It involves the use of medications to help patients relax, with various levels of sedation available depending on the patient’s needs and the complexity of the procedure. Sedation dentistry reduces anxiety, allows for more efficient treatments, and improves the overall patient experience.
